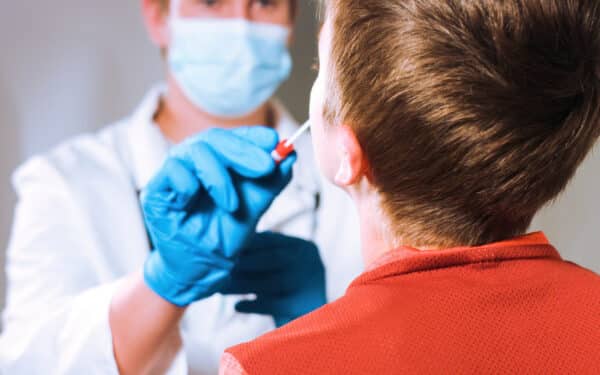
The Health Secretary says that the NHS must reduce maternity deaths and injuries by learning lessons, but yet again he’s saying something agreeable while avoiding accountability.
Year on year, the NHS is responsible for an unusually high rate of avoidable deaths compared to its peers. Its cost of malpractice also is high relative to peers: in fiscal year 2016-2017, the NHS paid more than £1.7 billion in damages and costs for clinical negligence, up from £1.5 billion in the previous year.
Why is Jeremy Hunt suddenly focused on learning lessons from maternity risks? He is perhaps belatedly compensating for unauthorized revelations in August that English maternity wards temporarily closed 382 times in 2016 – a record in recent years. The National Childbirth Trust previously reported that mothers in labour are being “treated like cattle” in NHS wards: half are left alone for hours without care or painkillers. The report’s authors – in consultation with the professional groups – chose to blame understaffing. Hunt’s new statement admits that staff numbers must increase. In immediate reaction to Hunt’s statement, journalists on BBC Radio 4’s Today Programme and a representative from the Royal College of Midwives blatantly colluded to discuss understaffing as the only issue.
What everybody involved agrees to avoid is structural accountability for malpractice. Hunt says all unexplained maternity cases should be investigated “independently” so that “lessons can be learned” without “blame,” but British healthcare is already subject to more than 70 nominally “independent” investigative organizations (by Parliament’s own count), and the lessons are always the same, but never learnt.
Currently, hospitals investigate themselves; if patients are unhappy, they can raise a complaint to one of those “independent” organizations or start civil legal action. Increasingly, patients go straight to legal action, given the frustrations and biases of officially “independent” organizations – whose dominant incentives are to avoid work and to protect the government and/or the professions that they represent, resource them, and staff them. The other term used officially for these organizations is “arms-length” – that’s not the same as “independent,” but since neither term is legally defined, these terms are used unaccountably.
The self-interests can be appreciated from the fact that the Parliamentary Health Services Ombudsman (PHSO) – the ultimate “independent” body for any complainant – investigated less than 8% of complaints in peak year, or merely 2,199 complaints; NHS England alone received 175,000 complaints that year. In the most recent year, the number of complaints rose, but the PHSO’s rate fell below 5%. According to heart-breaking testimonials, the other 95% are treated by PHSO staff as time-wasters, liars, idiots, fantasists, egotists, and objects of ridicule.
This is not an undiscovered problem, it’s an officially ignored problem: the PHSO has been the top of the pile since 2009, the anti-PHSO pressure groups date from around then, Jeremy Hunt has been Health Secretary since 2012, I have been reporting the structural explanation for Britain’s high health risks since 2013, and the Public Administration Select Committee has complained since 2015 that the PHSO is practically unaccountable to Parliament.
Yet here we go again: Hunts promises more “independent” “lessons-learning.” Hunt says that the Healthcare Safety Investigations Branch (HSIB), which became effective in April, should investigate all cases of unexplained serious harm during maternity care, but it is resourced to investigate 30 cases per year, when about 1,000 babies per year unexpectedly die or are severely brain damaged in Britain during maternity.
Hunt says the HSIB is “independent,” but the HSIB is not independent: it is funded by the Department of Health and sits within a department called NHS Improvement.
Hunt’s new statement on maternity risks went on: “We have to change a blame culture into a learning culture.” In fact, we don’t have a blame culture, because none of those “independent” organizations blames individuals. So far as they ever reach judgements, these are to the effect that “mistakes were made,” but no person is held accountable. Focusing on culture is convenient because a culture is the attribute of a group, but is no person’s fault. The HSIB was set up explicitly to avoid “blame” in favour of “learning lessons” from a few exemplary cases – but this is contradictory, since selective and blame-less investigations cannot learn all the lessons.
More importantly, a system without blame is an unaccountable system, and unaccountable systems are riskier systems. Unless the persons who are the sources of health risks are accountable for health risks, health risks will continue to move in the wrong direction.
Accountability should start with the government. If the Department of Health were to be made responsible for investigating the hundreds of thousands of complaints made against British health and social care per year, and were to be made accountable to Parliamentary committees for reducing health risks, our health risks would soon improve. Britons are dying for accountability.
Bruce Newsome is a Lecturer in International Relations at the University of California Berkeley